Let me preface this post by sharing that I’m not someone who drinks, particularly when I heard of the WHO consensus statement in 2023 that there is no level of alcohol that is safe for consumption (in contrast to the often echoed guidelines about how men and women should consume under two and one standard drink(s) daily). This is similar to how there is no level of cigarette smoking that is safe. Nevertheless, alcohol consumption is extremely prevalent, and is commonly viewed as a means by which people in society can socialise more easily.
Starting medical school has a way of turning everyday experiences into mini science lessons. Let me share with you some of the details of ethanol metabolism that I learnt about as I studied biochemistry previously.
1. The biochemistry of ethanol metabolism
Ethanol is metabolized primarily through two key enzymes in a two-step process that happens mostly in hepatocytes (liver cells). First, alcohol dehydrogenase (ADH) oxidizes ethanol into acetaldehyde. This step reduces NAD⁺ to NADH. Acetaldehyde is a highly toxic substance and a known carcinogen. Your body doesn’t let it hang around for long, though. Next, aldehyde dehydrogenase (ALDH), particularly the mitochondrial ALDH2, quickly converts acetaldehyde into acetate (acetic acid). Acetate is then turned into acetyl-CoA and fed into the citric acid cycle, eventually becoming CO₂ and water. Consider the following diagram (a screenshot from a review book that I used extensively during medical school):
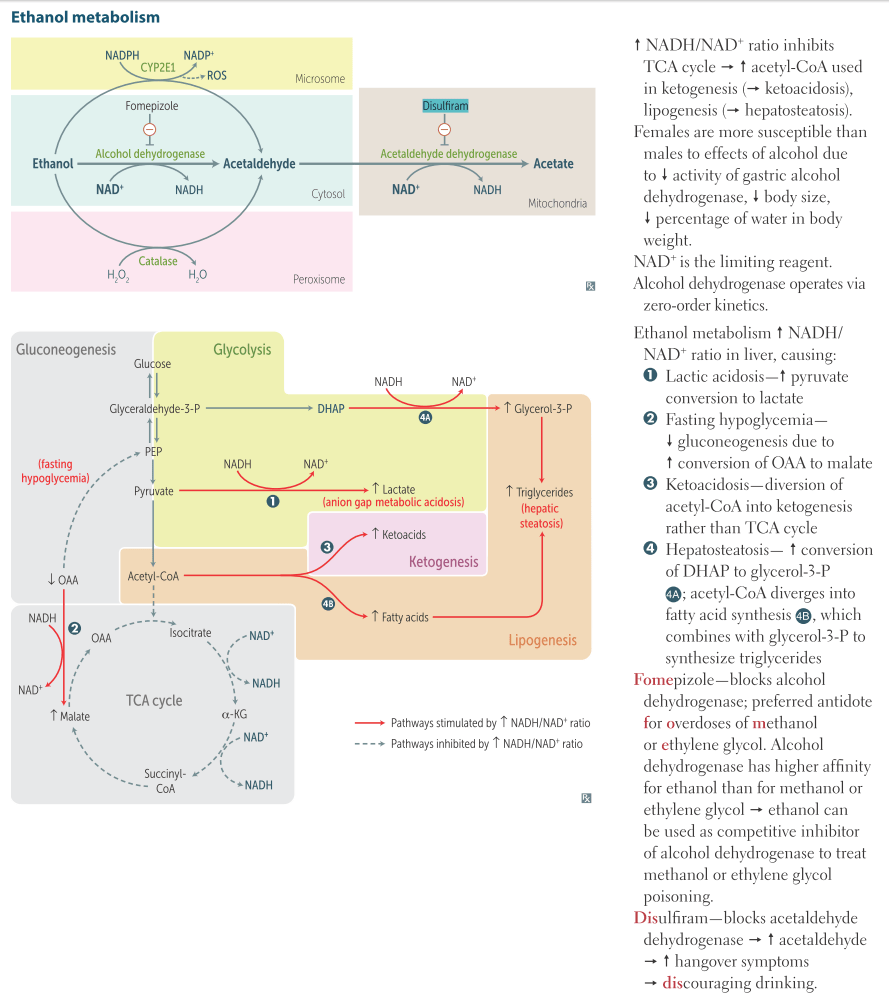
This above pathway is why our bodies can clear alcohol at a relatively steady rate (about 7–10 grams per hour on average, or roughly one standard drink), but it also explains a lot of the damage. The buildup of NADH shifts the cell’s redox state, which can mess with other metabolic processes, contributing to things like hypoglycemia or AFLD (alcoholic fatty liver disease) in heavy drinkers.
The real “wow” moment for me was learning about disulfiram (not something I see in clinical practice in Singapore, but interesting to learn about it; it’s probably something used in the US). This drug is used in alcohol dependence treatment and works by irreversibly inhibiting ALDH. If you drink while on it, seurm acetaldehyde levels skyrocket, often 5–10 times higher than normal. The result of drinking while on disulfiram is a disulfiram-alcohol reaction: flushing, nausea, vomiting, palpitations, headache, and a general feeling of impending doom. It’s basically weaponizing the body’s own hangover chemistry as aversion therapy.
I was astonished at how elegantly (and brutally) it targets that single step in the pathway of ethanol metabolism. It’s a reminder of how finely tuned our metabolism is, and how a small backup in the pathway can make you feel utterly miserable.
2. The gritty etymology of “hangover”
The second lesson came from outside the textbook. I recently came back from a trip to Japan, and whilst resting in the hotel rooms in the evening during the trip, I would sometimes watch some educational videos to expand my general knowledge. On one of the evenings, I had watched a video about the typical life of the underprivileged in Victorian-era London. The real story of the story behind the term ‘hangover’ is darker and more human.
In Victorian-era London, extreme poverty meant many destitute or homeless people couldn’t afford proper lodging. Apparently, for four pennies, you could buy a space on a very humble bed (whose sheets would not have been changed for a long time), and rest while supine. One could use such a space for eight hours and attempt to get some rest. However, some of the underprivileged, with their limited funds, would spend one or two pennies getting some alcohol instead, in an attempt to drown out their sorrows with the effects of alcohol at least in the form of a temporary escape. As a result, they wouldn’t have the required four pennies to rent a bed for eight hours. The result is that they aren’t able to afford the four-penny bed where they can lie down supine. Instead, they would have to opt for cheaper accommodation to spend the night.
For a lower price of two pennies, they could pay for a “two-penny hangover” in certain rough shelters. Proprietors would stretch ropes across a room like clotheslines. People would lean or drape themselves over these ropes to sleep—literally hanging over them. In the morning, the ropes were cut or lowered, and everyone “hung over” would drop to the floor, often still feeling the effects of cheap alcohol from the night before.
The Victorian image is vivid and poignant. It captures both the literal “hanging over” and the lingering misery that follows a night of drinking. It’s a stark reminder that hangovers aren’t just a modern inconvenience. They’ve been part of human (and especially underprivileged) experience for a long time.
Medical school has this habit of making the mundane profound. The next time you go out drinking with colleagues and friends (if you do drink), do consider the biochemistry churning away in your liver. Perhaps also spare a thought for those poor souls draped over ropes in 19th-century London…

Leave a comment